Dry Socket Symptoms: Warning Signs You Shouldn't Ignore After Tooth Extraction
Dry socket symptoms can transform a routine tooth extraction into a painful ordeal, affecting approximately 2% to 5% of all tooth extractions . However, this number jumps significantly with wisdom teeth removal, where dry socket lesions occur in up to 38% of mandibular third molar extractions . As dental professionals, we consider this the most common complication following tooth removals, particularly after wisdom teeth extraction .
The pain usually begins 1 to 3 days after the tooth removal , often radiating from the socket to your ear, eye, temple, or neck on the same side of the extraction . In fact, knowing the early signs of dry socket can save you from unnecessary suffering. These warning signs include severe pain that worsens days after extraction, bad breath, an unpleasant taste in your mouth, and sometimes fever . Therefore, understanding what dry socket looks like and when dry socket symptoms start is crucial for anyone who has recently undergone a tooth extraction.
In this comprehensive guide, we'll explain how to know if you have dry socket, what distinguishes it from normal healing, and what steps to take if you suspect you're experiencing this painful condition after tooth extraction.
What is dry socket and why does it happen?
After a tooth extraction, your body initiates a complex healing process that can sometimes go awry, resulting in a painful condition called dry socket or alveolar osteitis. This occurs when the protective blood clot either fails to form, becomes dislodged, or dissolves prematurely, leaving the bone and nerves exposed.
How a normal socket heals after extraction
Initially, a blood clot forms in the empty socket where your tooth was removed. This clot serves as a protective layer over the underlying bone and nerve endings, containing cells essential for proper healing [1]. Under normal circumstances, this clot remains in place for 7 to 10 days, performing crucial protective functions before dissolving naturally as new tissue replaces it [2].
During this period, granulation tissue—a creamy white mixture of collagen, white blood cells, and blood vessels—forms to cover the wound and facilitate healing [3]. Subsequently, the gums close over the socket while the bone underneath undergoes a remodeling process that takes several months to complete [4].
What causes the blood clot to dislodge
The blood clot can become dislodged for various reasons. Common culprits include:
- Smoking and tobacco use—chemicals in cigarettes can prevent healing, while the sucking motion may dislodge the clot [1]
- Creating suction in your mouth through activities like drinking through straws [3]
- Improper oral hygiene or not following post-extraction care instructions [1]
- Bacterial contamination from food particles entering the socket [5]
- Trauma during a difficult extraction, especially with impacted wisdom teeth [1]
- Playing with the extraction area using your tongue [3]
Why exposed bone leads to pain
Once the bone becomes exposed, intense pain follows—the hallmark symptom of dry socket [1]. This occurs because the protective layer that should cover the bone and nerve endings is missing, allowing direct stimulation of the nerve endings [5].
Besides pain, exposed bone can lead to additional problems. Food particles may get trapped in the socket and ferment due to bacteria, producing toxins that further irritate the bone [5]. This process also creates an unpleasant taste and halitosis (bad breath) [5].
Consequently, the pain from dry socket typically radiates from the extraction site to your ear, eye, temple, or neck on the same side [6]. Many patients describe this as a steady, throbbing pain that's severe enough to disrupt daily activities and often doesn't respond well to over-the-counter pain medications [6].
Early symptoms of dry socket you should watch for
Recognizing the warning signs of dry socket early can save you considerable pain and complications. Unlike normal post-extraction discomfort that gradually improves, dry socket symptoms worsen over time and require prompt attention. Let's explore the telltale signs you shouldn't ignore.
Pain that worsens 1 to 3 days after extraction
The most distinctive symptom of dry socket is severe, throbbing pain that begins 1 to 3 days after your tooth extraction [7]. This timing is critical—while some discomfort immediately following extraction is normal, pain that intensifies rather than improves by the second or third day signals trouble [1]. Moreover, dry socket pain is typically more intense than ordinary post-extraction soreness [6]. This pain persists and worsens over time rather than gradually improving as expected during normal healing [6].
Bad breath or foul taste in the mouth
An unpleasant taste in your mouth that doesn't go away with brushing or rinsing often indicates a dry socket [1]. This occurs because bacteria multiply in the empty socket where food particles can break down [6]. The resulting bad breath or foul odor [7] stems from bacterial infection at the extraction site [8]. Notably, if these symptoms persist despite good oral hygiene, they strongly suggest your socket isn't healing properly [1].
Visible bone in the socket
In normal healing, a dark blood clot covers the extraction site. With dry socket, however, you might notice an empty-looking hole where your tooth was removed [7]. First thing to remember is that a healthy socket should never show exposed bone. If you can see whitish or grayish bone in the socket [1], that's exposed jawbone—the primary cause of your pain [9]. This visual confirmation often helps distinguish dry socket from normal post-extraction discomfort.
Pain radiating to ear, eye, or neck
The pain from dry socket rarely stays localized. Instead, it commonly radiates to your ear, eye, temple, or neck on the same side as the extraction [7][10]. This spreading pain pattern occurs because exposed nerve endings trigger radiating pain signals [1]. The discomfort may feel like it covers the whole side of your mouth or face [11], sometimes described as intense, sharp pain similar to nerve pain [8].
How to tell if it’s dry socket or normal healing
Distinguishing between normal healing and dry socket after a tooth extraction can be challenging for patients. Accurate identification helps ensure proper treatment and prevents unnecessary suffering.
What does dry socket look like?
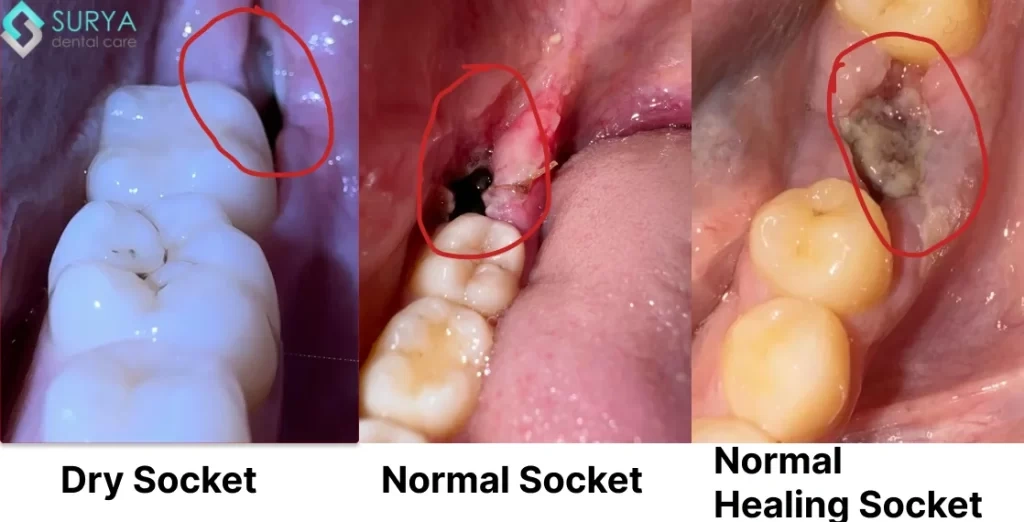
A healthy healing socket appears as a dark red blood clot filling the extraction site. In contrast, dry socket reveals an empty-looking socket where bone is visible. You'll notice a whitish-gray color at the bottom of the socket—this is exposed bone. The surrounding gum tissue often appears inflamed and may show signs of infection. Unlike a healthy extraction site that gradually fills with granulation tissue, dry socket lacks this protective covering.
Signs of dry socket vs. normal post-extraction pain
Normal post-extraction discomfort:
- Gradually decreases after the first day
- Responds well to over-the-counter pain medication
- Bleeding stops within 24 hours
- Mild swelling that peaks at 48-72 hours
Conversely, dry socket indicators include:
- Pain that intensifies rather than diminishes
- Discomfort unrelieved by prescribed medications
- Persistent bad breath despite good oral hygiene
- Pain radiating to your ear, temple, or neck
When do dry socket symptoms start?
Typically, dry socket symptoms emerge 1-3 days following extraction. This timing is significant since normal post-extraction pain should be improving by this point. Although discomfort immediately after extraction is expected, pain that suddenly worsens after this initial period strongly suggests dry socket. Altogether, if symptoms persist beyond the third day or intensify rather than improve, contact your dentist promptly.
What to do if you suspect dry socket
Prompt action is crucial if you suspect dry socket to prevent unnecessary pain and complications. Here's what you need to do and what to expect.
When to call your dentist
Contact your dentist immediately if you experience increased pain that doesn't respond to medication, especially if it keeps you up at night [3]. Other warning signs include visible bone at the extraction site, persistent bad breath, or a foul taste in your mouth [4]. Should you notice any symptoms of infection such as fever or swelling, seek professional care without delay [11].
How dentists diagnose dry socket
Dentists primarily diagnose dry socket through visual examination of the empty socket [9]. They'll check for exposed bone and absence of a blood clot [4]. In some cases, your dentist may take X-rays to ensure no tooth fragments remain in your jaw that could be causing the pain [9].
Treatment options: dressings, rinses, and pain relief
Treatment typically involves cleaning the socket to remove food particles and debris, followed by placing medicated dressings containing numbing agents like lidocaine or eugenol [3]. Your dentist may prescribe antibiotics if infection is present [3]. For pain management, over-the-counter medications like acetaminophen (Tylenol) and ibuprofen (Advil) often work better than prescription opioids when taken together [3]. Salt water rinses (½ teaspoon salt in 8 ounces warm water) can help eliminate bacteria [12].
How long does it take to heal?
With proper treatment, dry socket generally heals within 7-10 days [9]. Pain usually subsides significantly within 24 hours after professional treatment [13]. Complete healing and tissue regeneration might take several weeks depending on the severity and your body's natural healing ability [2].
Conclusion
Dry socket represents a painful complication that affects a small percentage of tooth extractions, though wisdom tooth removals face significantly higher risks. Understanding the warning signs certainly makes all the difference between unnecessary suffering and prompt treatment. The absence of the protective blood clot exposes sensitive nerve endings and bone, resulting in that characteristic intense, radiating pain that typically begins 1-3 days after extraction.
Recognizing the difference between normal healing discomfort and dry socket symptoms proves essential. While regular post-extraction pain gradually improves, dry socket pain intensifies over time. Additionally, visible bone in the socket, persistent bad breath, and pain radiating to your ear, eye, or temple strongly indicate this condition rather than normal healing.
Should you notice these warning signs, contacting your dentist immediately remains your best course of action. Most dental professionals can diagnose dry socket through visual examination and provide effective treatment through socket cleaning and medicated dressings. The good news? With proper care, relief usually comes within 24 hours, and complete healing takes place within 7-10 days.
Prevention stands as your strongest defense against this painful condition. Following post-extraction care instructions carefully helps protect that crucial blood clot. Avoiding smoking, straws, and excessive spitting significantly reduces your risk. Therefore, vigilance during those first few days after extraction, combined with proper aftercare, helps ensure your tooth extraction experience remains as comfortable and complication-free as possible.
Key Takeaways
Understanding dry socket symptoms can help you distinguish between normal healing and a serious complication that requires immediate dental attention.
• Watch for worsening pain 1-3 days post-extraction - Unlike normal healing pain that improves, dry socket pain intensifies and radiates to your ear, eye, or neck.
• Look for visible bone and persistent bad breath - An empty socket showing whitish-gray bone instead of a dark blood clot, plus foul taste despite good hygiene, signals dry socket.
• Contact your dentist immediately if symptoms worsen - Professional treatment with medicated dressings typically provides relief within 24 hours and full healing in 7-10 days.
• Prevention is key to avoiding this painful condition - Follow post-extraction care instructions, avoid smoking and straws, and protect the blood clot during the first few critical days.
Remember, dry socket affects only 2-5% of extractions but can occur in up to 38% of wisdom tooth removals. Early recognition and prompt treatment prevent unnecessary suffering and ensure proper healing.
FAQs
Q1. How soon after tooth extraction can dry socket occur? Dry socket symptoms typically appear 1 to 3 days after tooth extraction. If you experience worsening pain or discomfort after this period, it may indicate dry socket.
Q2. What does dry socket look like compared to normal healing? A dry socket appears as an empty-looking socket with visible whitish-gray bone, while a normally healing socket has a dark red blood clot covering the extraction site.
Q3. Can dry socket heal on its own without treatment? While dry socket can eventually heal on its own, it's best to seek professional treatment to alleviate pain and prevent complications. Proper treatment can significantly reduce healing time and discomfort.
Q4. How is dry socket treated by dentists? Dentists typically clean the socket, remove debris, and apply medicated dressings containing pain-relieving agents. They may also prescribe antibiotics if there's an infection and recommend pain management strategies.
Q5. What can I do to prevent dry socket after tooth extraction? To prevent dry socket, follow post-extraction care instructions carefully. Avoid smoking, using straws, and excessive spitting. Maintain good oral hygiene and protect the blood clot during the first few days after extraction.
References
[1] - https://impressionsdental.com/blog/how-to-tell-if-you-have-early-stage-dry-socket-or-dry-sockets/
[2] - https://inlandchoicedental.com/dry-socket-5-days-after-wisdom-teeth-extraction/
[3] - https://www.health.harvard.edu/diseases-and-conditions/dry-socket-preventing-and-treating-a-painful-condition-that-can-occur-after-tooth-extraction
[4] - https://www.dentistryofwestbend.com/dry-socket-diagnosis-treatment-and-more/
[5] - https://pmc.ncbi.nlm.nih.gov/articles/PMC5932271/
[6] - https://www.familydentalcare.com/how-do-i-know-if-a-dry-socket-alveolar-osteitis-is-forming/
[7] - https://www.mayoclinic.org/diseases-conditions/dry-socket/symptoms-causes/syc-20354376
[8] - https://www.greatbasinofs.com/dry-socket-after-wisdom-teeth-removal/
[9] - https://my.clevelandclinic.org/health/diseases/17731-dry-socket
[10] - https://medlineplus.gov/ency/patientinstructions/000780.htm
[11] - https://www.healthline.com/health/how-long-does-dry-socket-last
[12] - https://www.healthline.com/health/home-remedies-for-dry-socket
[13] - https://www.emergencydentistofaustin.com/blog/is-dry-socket-a-dental-emergency





